After a rocky start and calls of foul from agents and brokers, changes to the federally-facilitated marketplace, commonly known as Healthcare.gov, are leading to an increase in the number of agents and brokers now selling through the exchange.
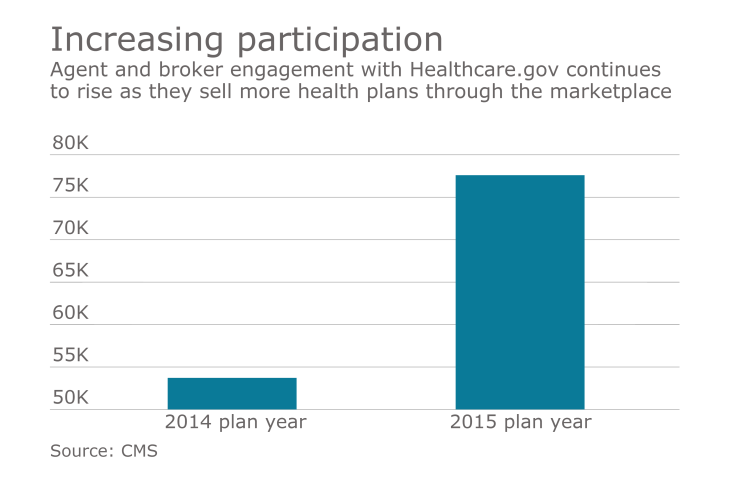
For 2015 open enrollment, more than 77,000 brokers and agents assisted with enrollments on the federally-facilitated marketplace, up 46% from the year prior.
Looking at the next open enrollment, there has been a “noticeable increase” in the number of agents and brokers participating as a result of more familiarity, says Marcy Buckner, vice president of government affairs at the National Association of Health Underwriters. According to Buckner, the Centers for Medicare and Medicaid Services has indicated to NAHU that the number of people going through agent and broker training has increased leading into this year’s open enrollment.
“The first year had a rocky rollout and some agents were hesitant to get involved on the exchanges,” she explains. “Since then, we have seen an increase in the number of [NAHU] members getting involved and going through certification,” which is required to sell on the exchange.
“Agents saw the stumbling blocks of the first two years and now feel more comfortable with the system,” she adds.
CMS changes
CMS recognizes the value agents and brokers bring to the marketplace, says agency spokesperson Aaron Albright. “Agents and brokers are an important part of enrolling eligible individuals who wants to get coverage,” he adds. “Whether through Healthcare.gov, the call center, navigators, or direct enrollment through an agent or web broker, consumers have many channels to choose from most convenient to them.”

Repeal the ACA. Build upon health reform. Increase consumer choice. Eliminate monopolies. The two candidates are divided on some policy, but there is also common ground in their proposals.
CMS and the Department of Health and Human Services are also conducting proactive outreach with agents, and “we really see the administration is reaching out and is interested in their involvement,” NAHU’s Buckner says.
Healthcare.gov CEO Kevin Counihan and his staff are listening to agent concerns, says B. Ronnell Nolan, CEO of agent lobbying group Health Agents for America. “[CMS] is … working with us to find solutions” to issues.
Working with CMS “really has turned,” adds Buckner. There is “more open dialogue then in the past couple of years.”
Also see: "
She explains that since the rocky rollout, CMS has made multiple improvements to help agents. Those include making it easier for consumers to find agents and brokers. Previously, it was difficult to find that information. “Now [agents] are listed in the same manner as other in-person assisters, such as navigators,” Buckner says.
Other issues that have been addressed by CMS include:
- National producer numbers falling off applications. “When we brought that up to HHS, it took them a bit of time, but they continually reported what was happening,” Buckner says. CMS discovered a glitch and fixed it. “It is no longer happening, which is huge for our folks because it is not only how they are paid but also a consumer protection to be able to see who is working with them,” she says. This is a major concern to ensure brokers are getting paid for their work, Nolan says. “Our tendency is to help people, regardless, we cannot work for free,” she adds.
- People at the call centers have been trained on “simple” agent and broker issues. “They are more familiar with how agents and brokers are registered,” Buckner says.
- Agents and have brokers now have their own newsletter from CMS, similar to what navigators and in-person assisters received since launch.
- CMS is also doing a lot more training and webinars for agents and brokers.
- CCIIO has a bi-monthly call with broker organizations “to touch base and hear what CCIIO is working on and we talk about some patterns we are hearing from members,” Buckner says.





