Many consumers are still unprepared for increased responsibility in their healthcare plans, a report released this week by consumer funding platform Alegeus finds.
As many employees continue to face rising deductibles and out-of-pocket costs, some are unsure of how to navigate choosing benefits and saving for healthcare. Consumers, on average, are more able to calculate the value of buying things such as a television or a car than costs crucial to their health — and retirement and emergency savings funds still take precedence.
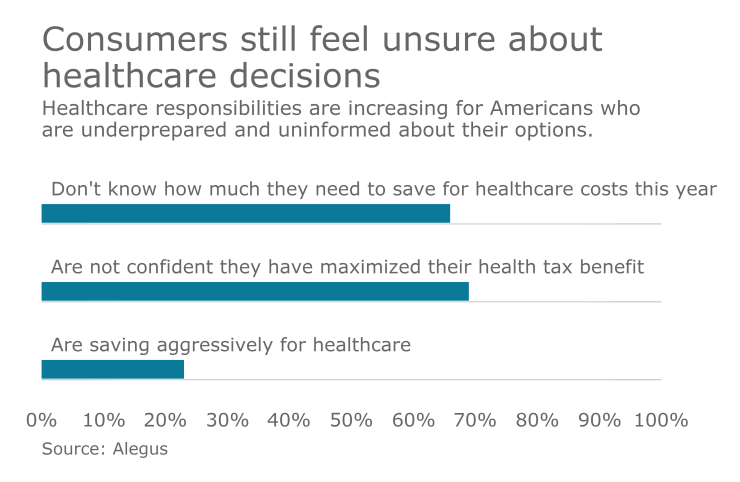
Of the more than 1,000 healthcare consumers surveyed for the report, 66% said they don’t know how much they need to save for healthcare costs this year, and only 23% are aggressively saving for healthcare. While 76% of consumers say they are focused on getting the best value for their healthcare dollars, almost 70% are not confident they have maximized their tax benefit for healthcare savings.
“The consumer index continues to reconfirm the critical need to help the average U.S. consumer get better support around managing their healthcare dollars,” says Steve Auerbach, CEO of Alegeus.
Adviser education
He says employers and benefit advisers can play a crucial role in changing this. Because much of this unpreparedness stems from a lack of education about healthcare and savings, advisers can be a tool to get consumers knowledgeable and engaged. This should be an ongoing process — not a short, once a year event.
“Most benefit advisers view healthcare as an annual event, but consumers use healthcare all year long,” Auerbach says.
Advisers should have multiple check-ins throughout the year, and personalize these check-ins to the consumer. Using platform technology, advisers can analyze the different needs between a millennial just out of college and someone starting a family.
Modern technology can also be used to reach out to consumers in multiple ways — via text, email or whatever seems to be the most effective for engaging a certain individual.
“Benefit advisers are in a unique position now because tools used to help their customers have rapidly advanced,” Auerbach says. “They have the opportunity to build trust with the consumer and personalize communication and messaging.”





