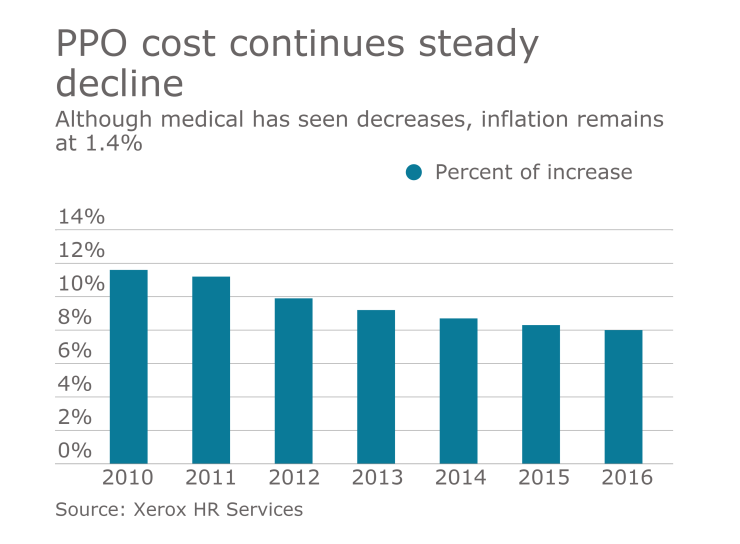
Choosing the right medical coverage can be a daunting task, especially for those who suffer from chronic illnesses or have a large family. Xerox HR Services recently released its 32nd National Healthcare Trend Survey and found that since 2010 healthcare costs have dropped from 11.6% to 8%. Despite this drop, when compared to the inflation rate, cost still maintains a wide lead above inflation, which the United States Bureau of Labor Statistics says is sitting at 1.4%.
This wide gap between cost and inflation has caused many employers to shift more cost over to employees. This has resulted in some consumers weighing price into their decisions of where and when to seek healthcare, and even delaying treatment due to cost.
Also see: “
“While it’s promising to see a slowing of increases, healthcare cost increases are still eating into employer revenue and employee paychecks at four or five times the rate of inflation,” says Harvey Sobel, principal and consulting actuary at Xerox. “Plan sponsors should remain vigilant, reviewing all facets of their medical plans, including benefit design, networks and vendors, to make sure they and their employees are getting the best value for the price.”
Some of the reasons medical cost continues to stay higher than inflation are due to use of diagnostic tests and treatments, limited reimbursement to providers from Medicare and Medicaid, mandated coverage of certain benefits, such as expanded mental health benefits and prosthetic legislation, increased administrative costs associated with new regulations, and up-front costs associated with new medical technology and treatments, according to the Xerox study.
Prescription medication
Prescription drug cost is another avenue of healthcare that is not seeing a reduction. Many Americans have seen this topic as one of the core subjects in the current presidential race between Hillary Clinton and Donald Trump. With the projected rate of increase rising from 6.7% in 2010 to a current 8.8%, respondents to Xerox’s study cited three key reasons for the rise.
First, the continued impact of specialty drugs, where, as an example, treatment for multiple sclerosis can cost more than $50,000 a year. Second, an increase in the number and use of pharmaceutical products that improve the quality of life and enhance lifestyles. And third, a dramatic increase in the number of expenses of compound pharmaceuticals.
“While specialty drugs continue to be a major component of prescription drug trend increases, there is a sizeable expense related to specialty medications billed under the medical benefit,” says Robert Ferraro, principal in the national pharmacy practice of Xerox. “Plan sponsors have an opportunity to save money by making sure these non-oral medications are administered at the appropriate site of service.”
Also see: “
Dental and vision are no exception
The survey also reported trend factors for dental and vision plans, with both showing lower and steady rates of cost increase. Between 2007 and 2016, dental plans have seen a decrease from 6.9% to 5%, while vision plans have seen a decrease from 3.6% to 2.9%.
Sobel says he has seen some companies offering dental included with major medical on individual health exchanges, but not to the point that it has taken off as a trend.
“Dental coverage usually covers a lot of preventative treatment, but because the Affordable Care Act, we have seen companies offering health insurance on the individual health exchanges that do have to cover dental for newborns and pediatric dental,” says Sobel. “That’s sort of coverage where we are seeing medical plans offering dental but I don’t think I’ve seen it take off as a trend, not to say it couldn’t.”
Shawn Jenkins, CEO of Benefitfocus, said in his final thoughts of the company’s 2016 State of Employee Benefits – Large Employer Edition, that it is reports like this and others like the one provided by Xerox that are giving advisers, brokers and employers the necessary information to educate themselves on the state of benefits in the U.S. and to make an informed decision on how to prepare their clients and staff for future obstacles.
“As we see from the data, employers recognize that to continue to provide the protection their employees need during this time of industry disruption, they must make fundamental shifts in their benefits offerings,” Jenkins says. “Many have experienced success in shifting costs and creating a consumer-driven healthcare model by offering HDHPs along with traditional plans, some even going as far full replacement. These consumer-centric benefit strategies are not only being well received by the workforce, specifically millennials, but they are also shielding large employers from impending taxes and penalties — no matter what form they may eventually take.”





