When an employee of Hill Country Memorial Hospital developed chronic kidney disease, the not-for-profit hospital in Fredericksburg, Texas faced a whopping bill. Not only was an employee facing a lifetime of dialysis treatments three times a week, missed work hours and increased medical care, the 80-bed hospital had maxed out its $1 million premium for its employee health plan.
“It cost us quite a bit,” recalls Becky Laughlin, the current benefits manager, who was the benefits coordinator at Hill Country Memorial Hospital when the incident occurred.
The hospital, located roughly 60 miles from Austin, had never exceeded its employee medical plan limit before. While Laughlin doesn’t recall when the patient began dialysis treatment, the ACA, which was signed into law in 2010, was not yet in effect.
After the episode, the HR and benefits team looked for a solution. They found one in data management provider Advanced Plan for Health, which oversees its employee medical care expenses generated by its third-party employee benefit administrator WebTPA. Using its Poindexter program, APH oversees the hospital’s employee medical expenses, looks for patterns of cost overruns, pharmaceutical pricing and possible drug seeking behavior, overuse of emergency room and urgent care facilities. It generates reports that are sent to employers on a weekly, monthly or quarterly basis.
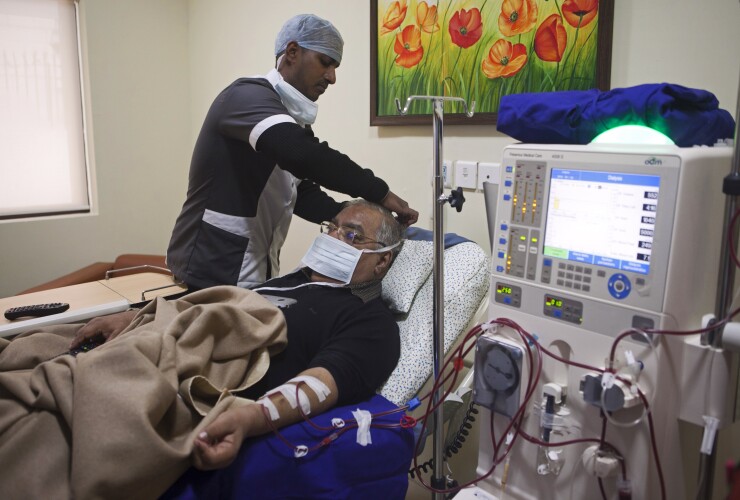
The hospital uses Poindexter to identify kidney disease among its 650 employees and dependents in order to predict the costs for kidney disease care and possible events such as heart attacks and the need for hospitalization. The app analyzes employees’ medical data to warn if a worker or family member is at risk of kidney failure and other diseases. If an employee is at risk, APH offers a nurse care management program to prevent dialysis and other treatments in the case of kidney disease.
Employers ignore kidney disease care at their own peril, says Dr. Barbara Rutkowski, vice president of clinical operations for AHP.
Instances of chronic kidney disease are growing, and late stage renal failure that requires dialysis and eventual transplants are on the rise. Nearly 10% of Americans over the age of 20 have some form of chronic kidney disease that’s on the continuum from very little to kidney shut down, which is end-stage renal disease.
“And it grows every year by about 5%,” warns Rutkowski.
Like other chronic conditions such as obesity, poor diet and sedentary lifestyles, employers often overlook kidney disease, instead focusing on heart attacks and strokes.
“People are not taking care of their diabetes, they’re not watching their weight and they’re not controlling their blood pressure, which is a huge factor,” she says. She adds that blocked arteries and capillaries from hypertension does damage to otherwise healthy kidneys.
“Our goal is to avoid the $350,000 to $700,000 per member per year that an employer will pay when somebody’s on dialysis,” says Rutkowski.
Besides the expense of dialysis treatments, Rutkowski says patients often lose three half days each week traveling to and from dialysis centers for their treatment.
“Can they work the second shift?” she asks.
Patients with renal issues also have co-morbidities like diabetes, heart disease and hypertension which can prompt a medical insurer to “laser” or point out potential employees who are at risk of exceeding an employer’s medical health plan premiums.
“You can compare it to car insurance: the higher the stop-loss of the group, the lower your premium for reinsurance or for another insurance company to kick in,” Rutkowski says.
An employer can often afford an employee’s $150,000 or $200,000 medical care, but insurers may “laser” in on one or two people in the plan who will then have a fixed cost. “Sometimes people on dialysis develop Stage 5 renal disease and they fall into that category,” Rutkowski says. Their expenses could reach $400,000 before the employer’s health plan’s reinsurance kicks in.
Rutkowski says Poindexter and its other services are being used by employers across the country and covers around 2.5 million lives.
Poindexter looks at an employee’s insurance claims, their number of hospital visits, and use of a primary care physician and how often they have had a urine analysis, for example. With this information, APH can create a plan of action so that the employee doesn’t need extensive kidney care and an eventual transplant. (The offering also looks at heart disease and other chronic illnesses.)
“We get three to four years of data so we can look at the trends and see the chronic conditions and the behavioral patterns,” Rutkowski says. “Behavior is very important; if they have six to nine people prescribing drugs there’s going to be a problem because communication starts to be an issue.”
Laughlin says the hospital uses APH as a “data warehouse.” “They help us figure out what's going on in our plan and provide reports on priority basis to see how we're using the plan, where we can make some improvements,” she says. “They can give us some valuable information so that we know how to where we can maybe improve our plan or what's working what's not.”
Laughlin warns that employers should be aware of the impact of the cost of kidney disease on their health plans.
“It can be so detrimental not only to the patient and their families but it can be hard on your health plan as far as cost,” she says. “If we have another person that needs these kind of services, there's something in place that we are now able to manage the cost of the treatment.”





