Is affordable group health insurance so difficult for small businesses to find that they’re better off steering employees to the individual market, farming out the administration and compensating their brokers or advisers as such?
The answer isn’t exactly cut and dried.
At the heart of this question is a bold claim that so-called
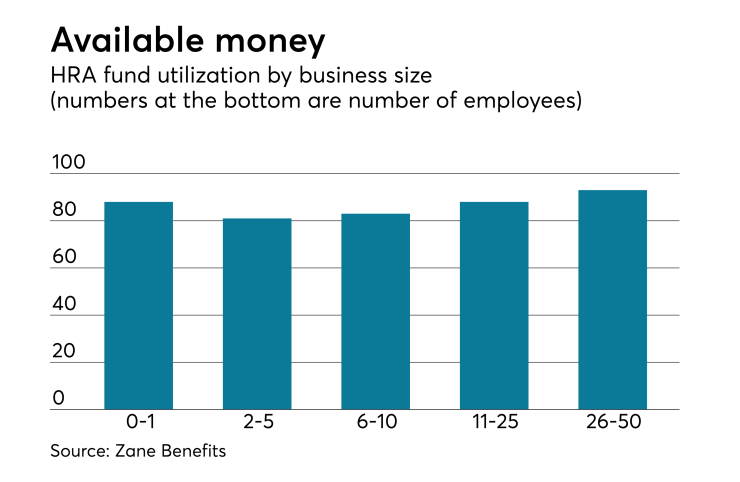
The report, which draws on data from more than 15,000 reimbursement plan participants, also highlights a 45% increase in HRP participation since 2015 and promotes the new small business health reimbursement arrangement plan created by Congress in December 2016. In fact, Zane now recommends this new type of HRA over the HRP because of its ability to reimburse medical expenses in addition to premiums.
An HRP provides allowances for employees that are used toward eligible healthcare expenses in the individual market. Here’s how it works: small businesses earmark a fixed amount of monthly funds to reimburse employees for individual health insurance and other medical expenses rather than select a group plan and pay a portion of the premium.
Although HRPs and HRAs are both Section 105 plans, the former “does not impose a plan-wide maximum annual benefit and does not allow annual roll-over,” according to Zane. The consulting firm adds that for some employers “a stand-alone HRA is no longer a compliant vehicle for premium reimbursement because of the new Affordable Care Act ‘market reforms.’”
And unlike a health savings account or flexible spending account, there’s no minimum or maximum limit to the amount of money an employer can contribute to an HRP.
The end of employer-provided health insurance?
“We need to blow up the employer model and get consumers buying individual health insurance, and if we want to give them federal tax credits, then great,” suggests Rick Lindquist, CEO and president of Zane Benefits and the author of The End of Employer-Provided Health Insurance.
He hastens to add that employers also should have an ability to give employees money through these HRAs and HSAs to secure a more seamless transition for employees. “Once you do that,” he says, “then you can start dealing with the actual problem, which is the cost of healthcare.”
But the small-group market is actually thriving “because the rate volatility is very minimal now,” says Ron Goldstein, president and CEO of CHOICE Administrator. His rate increases have been lower than 5% in some cases. He believes brokers and advisers would need to write a high enough volume in the individual market to make it a worthwhile investment of time.
Also see: “
Moreover, Goldstein doesn’t consider the HRA employer deduction market as much of a homerun; just a small piece of the market into which he might dip his firm’s toe. “My gut says that it will not be as big of a disruptor as Zane is making it out to be because it’s been around,” he explains. “The only difference now is employer deduction.”
While Zane claims health reimbursement provides greater value, it’s actually in the eye of the beholder, says Mark Fendrick, M.D., professor of internal medicine in the University of Michigan’s School of Medicine and health management and policy in the School of Public Health. He’s unconvinced that health insurance coverage in the individual market will provide as much or greater value than on a group basis without seeing an apples-to-apples comparison that provides incontrovertible evidence to support that claim.
“It’s time to change our conversation on healthcare in the U.S. from how much we spend to how well we spend,” says Fendrick, who’s also co-founder and director of the University of Michigan Center for Value-Based Insurance Design.
Meanwhile, how do HRPs affect brokers and advisers?
The same census data they gather to assess group health plans can be used to decide whether or not an individual-market solution is better for a particular employee population, Lindquist says. Brokers then would outsource the plan to a partner that helps employees navigate the individual market or simply enroll each individual if they already offer that service in house. Zane has a partner program that features revenue sharing with brokers or adviser on the consultant’s fees.
What’s critical about these assessments is that they take into account the age of those employees, household size, home ZIP codes and income, he says, adding that the information can be used “to figure out what the right amount that then an employer might reimburse on a monthly basis.”
Ultimately, Lindquist observes, small businesses want is a recruiting and retention tool that unshackles them from a limited employer-provided healthcare system. He believes more of them “would welcome the opportunity to stop being the middleman and get more flexible with their employee benefit arrangements.”





