Diabetes should be at the top of every client’s priority list.
But navigating the complex world of diabetes management solutions can be challenging, and employers need to ask tough questions in order to determine which offerings are right for their workers.
More specifically, when assessing tools like a glucose monitoring device, employers need to think about whether it meets clinical best practices and lowers the cost of care. It also is important for employers to understand whether adding a device that allows employees to self monitor their blood glucose supports the treatment plan.
Evidence suggests that lifestyle changes like weight loss, adherence to medication, receipt of preventive care and self-monitoring of blood glucose can positively impact diabetes outcomes. These are all topics covered in diabetes self-management education and support (DSMES), an ongoing plan for diabetes care and a covered benefit under most health plans.
DSMES is provided to patients in a group or individual format and staffed by a single educator who works longitudinally with a patient. DSMES is shown to improve hemoglobin A1c (HbA1c), the primary metric used to monitor diabetes, by as much as 1% in people with Type 2 diabetes. The great thing about DSMES, and working with the same educator over time, is that the lessons are tailored for the needs of the individual patient.
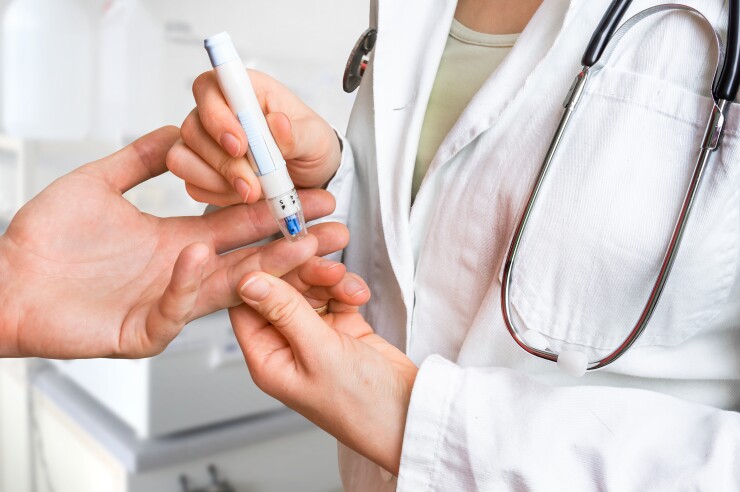
It’s also important to remember that not all patients need all services. For example, home glucose monitoring is not always clinically impactful or cost effective.
See also:
There is good evidence that checking blood sugar for those with Type 1 or Type 2 diabetes on insulin or certain oral medications is important. But for the majority of patients with Type 2 diabetes, those not on insulin, the evidence is inconclusive at best. The American Diabetes Association does not recommend self monitoring of blood glucose for those with Type 2 diabetes on oral medications unless the provider prescribes it. This is a practice also supported by the Centers for Medicare and Medicaid Services for Medicare beneficiaries.
Whether or not a diabetes patient should be engaging in self-monitoring is a decision between patients and their physician. First, an employee’s care team may decide to focus on lifestyle change or preventing complications instead of glucose monitoring. If monitoring is needed, an individual may already have a preferred device and you as an employer may have an existing relationship with a specific vendor. For many patients with diabetes, especially those with Type 1 diabetes, use of a continuous glucose monitor has become standard of care. Blood glucose meters, or finger-stick meters, are cumbersome for patients who check multiple times a day.
Patients become comfortable with a specific monitoring approach over time and often prefer to continue with the device that they are used to. Your health plan may also have a preference for which type of monitoring should be recommended. Most importantly, the doctor may also have a preference. Many providers are now leveraging data integrations with specific glucose meters to facilitate more comprehensive care. A personalized approach to diabetes care needs to include flexibility around monitoring devices.
Many companies rely on artificial intelligence-based outreach to promote behavior change instead of investing in personalized coaching. This investment misdirects resources towards devices and flashy data platforms, as opposed to proven behavior change techniques. Behavior change requires a longitudinal individual coach and group support to set goals and provide accountability. These services can be enhanced with technology, but it should never replace people.
So why don’t more employers take a personalized approach to diabetes care? One possibility is that it’s cheaper and easier to scale an intervention that doesn’t change with the participant. If you’re charging based on devices and strips dispensed, there is no incentive to personalize. But as the market matures, more employers will demand that program costs are linked directly to clinical outcomes and participant engagement.
Given the central need for behavior change in diabetes, a device-forward approach means thoughtfully incorporating devices when they support behavior change, impact outcomes and reduce costs. Placing technology ahead of the needs of patients is perpetuating the same issues that plague healthcare today — misaligned incentives that drive the overuse of unneeded or unproven therapies.





