Your client's workers and their family members frequently face tough questions about their healthcare: How do I know when it’s time to get a mammogram? When does my child need a vision screening? Should I get a thyroid screening? If I have high blood pressure or diabetes, what is the best treatment for me?
For the providers who care for them, the key question is: How do we implement appropriate, science-backed treatments for our patients, testing where needed, but avoiding potentially harmful or unnecessary (and expensive) care? The answer is to seek guidance from and use clinical guidelines —along with existing clinical skills — wisely.
Clinical guidelines are sets of science-based recommendations, designed to optimize care for patients in areas such as screening and testing, diagnosis and treatment. They are developed after a critical review by experts of current scientific data and additional evidence to help inform clinical decisions across a spectrum of specialties.
Based upon this process, guidelines are then released by a number of sources and collaborations, including academic and non-profit healthcare entities, government organizations and medical specialty organizations.
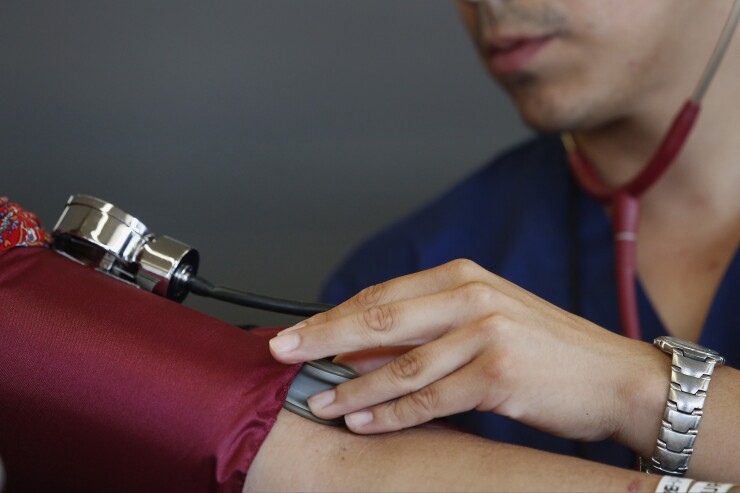
From preventive care to treatment protocols for chronic conditions, guidelines provide a framework healthcare providers use with patients to help guide care. However, it’s important to note that clinical guidelines are not rigid substitutes for professional judgment, and not all patient care can be encompassed within guidelines.
The impact on healthcare and benefits
Clinical guidelines are used in myriad ways across the healthcare spectrum, and providers are not the only ones who utilize them. Insurers also may use guidelines to develop coverage policies for specific procedures, services and treatment, which can affect the care your covered population receives.
To illustrate a key example of an intended impact of guidelines on health plan coverage, consider those issued by the U.S. Preventive Services Task Force, whose A and B level recommendations comprise the preventive services now covered at no cost under the mandate of the Affordable Care Act.
As another example, the National Committee for Quality Assurance, which accredits health plans and improves the quality of care through its evidence-based measures, uses the American Heart Association guidelines when creating its quality rules for treating high cholesterol with statin drugs.
Other examples exist among commercial coverage policies. For example, some cancer drug reimbursement policies use components from nationally recognized guidelines for cancer care.
Because science is rapidly changing, guidelines are often updated, leading insurers to revisit their policies to decide if they will change how services and medications are covered for their members. Providers and health systems may modify processes of patient care in response to major changes in guidelines and/or resultant changes in payer reimbursement.
Not all guidelines are updated on a set schedule, making it even more important for providers and organizations that rely on guidelines to stay on top of changing information, as it can have a direct impact on how they work. Attending conferences, visiting the recently established
Why it matters for employers
As employers or benefits consultants, it’s critical to ensure that your health plan, advocacy or decision support providers, and other partners that depend on this information to guide their practices and decisions understand and follow current, relevant guidelines.
Further, by combining information from relevant guidelines and data from biometric screenings, health risk assessments, claims and other sources, it’s possible for clinical advocacy and other decision support providers to identify employees with gaps in care and generate targeted communications (through a member website and/or mobile app) to help them take action to improve their health.
Clinical guidelines are science distilled into practical recommendations meant to be applied to most patients for quality healthcare. By maintaining current, relevant guidelines, organizations and providers who work with your covered population can ensure that all parties have the key information they need to make the best decisions for their health.





